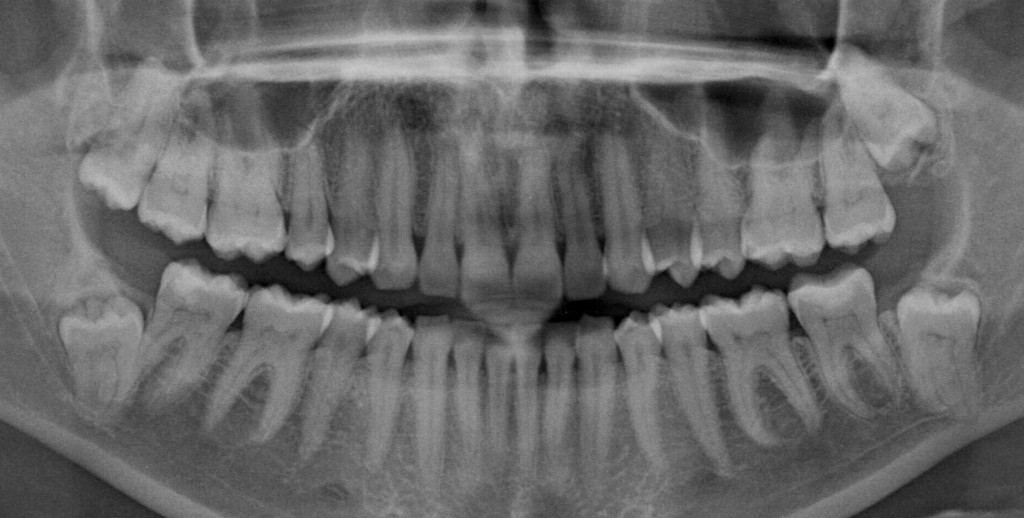
It is an unfortunate part of life that not all teeth will last forever. There are many reasons why eventually teeth will need to be removed (extracted) when all other options to repair them have failed, or are not realistic. Causes of tooth extractions include:
- Extensively decayed, broken, or cracked teeth
- Advanced periodontal (gum) disease
- Not suitable to root canal
- Poor long-term prognosis
- Non-functional (not in the bite) and over-erupting
- Malpositioned or impacted
- Replacement with prosthesis such as implants, bridges, or dentures
- Cost of dental treatment to save the tooth may be questionable, or unrealistic for the patient
- Removal as part of an overall medical treatment plan
During cancer treatment, some people receiving radiation to the head and neck may need to have ‘suspect’ teeth removed prior to the commencement of radiotherapy. Whilst others receiving chemotherapy may be at risk of developing infections from teeth that have poor gum support due to their weakened immune system. Other patients may have severe and unstable cardiovascular conditions such as heart disease or require heart bypass surgery and will have teeth removed to prevent post operative complications.
People receiving an organ transplant and immunosuppressive medications may also need some teeth extracted if the teeth are at risk of becoming sources of infection after the transplant.
Sadly, having a tooth or teeth removed can for many people be an incredibly traumatic and highly emotional experience for varied reasons such as pre-conceived thoughts, fears and phobias, concerns over aesthetics and function of their smile and bite after the extraction, previous negative experiences, a history of tooth ache and pain (either short term or chronic), other people’s “horror stories”, and simply (but very importantly) the person just does not want to lose a tooth.
Unforeseen complications and difficulties can sometimes occur no matter how well the planning of an extraction is carried out, or how well skilled the dentist or oral surgeon is when removing the tooth. Generally however, having a tooth (or teeth) removed should NOT be an ordeal, a traumatic experience for patients, or take excessive amounts of time. Generally, nearly all extractions are for the most part reasonably straight forward, even when they require surgical removal. Even complicated surgical extractions typically take no longer than 15 minutes per tooth. Most simple extractions take less than 5 minutes.
In addition, it is quite common for people to say they have been told or heard that they cannot have a tooth removed if there is an infection present. This simply is not all that true and most infections in the mouth are there because of the tooth or poor gum support. Remove the tooth, and you remove the infection. It is true that infections can make anaesthesia more difficult, but in general there are no teeth that cannot be removed because of an infection. In a large proportion of cases, leaving an infected tooth in the mouth and placing a person on antibiotics just prolongs a patients’ pain and can place them at risk of complications from the infection or the antibiotics.
Another misconception is that people on anticoagulant (blood thinning) treatment need to stop their aspirin or warfarin prior to having a tooth extracted. This practice can sometimes be quite dangerous for a patient whom is at high risk of cardiovascular complications should they cease their medications.
In our practice, blood thinners should not be ceased by the patient or on instruction by a GP prior to extractions or oral surgery without prior consultation with Dr Eldridge.
Treatment of patients taking ‘blood thinners’ is explained further under “Medically Compromised Patients”.
There are generally two types of extractions, and these are called “Simple Extractions” and “Surgical Extractions”.
Simple Extractions
Simple extractions are typically performed on a tooth that can be readily seen in the mouth and are commonly performed under local anaesthetic in the dental chair. Typically, simple extractions are performed with a pair of forceps and / or an elevator by applying slow and controlled pressure to the tooth until it becomes loose within the socket and can be elevated without difficulty. Simple extractions with experience generally can be performed in less than 5 – 10 minutes in most circumstances. More complicated extractions such as lower molar teeth, people with dense jaw bones, or teeth that are broken down, may take longer as more time is needed to very gently pry the tooth from its socket and prevent teeth from fracturing.
Having a tooth (or teeth) removed should not be an ordeal, or a traumatic experience.
Some extractions require ‘sectioning’ due to their root structure (shape), or they have little remaining coronal (top of) tooth structure remaining for application of the forceps or elevator. Or the patients bone is so dense, it is better to remove the tooth in portions rather than one piece. This is not a ‘surgical extraction’ but rather the tooth is drilled and a small amount of bone is removed to allow all portions of the tooth to be removed simply and without applying excessive pressure to the jaw and temporomandibular joints. Sectioning of teeth is quite commonplace and is better to be done sooner rather than later when a simple extraction is not going to plan. Sectioning a tooth is far easier and more comfortable for the patient (and dentist) than persisting with an extraction for 15 minutes or more and then realising the tooth is not going to come out in one piece.
Most simple extractions and sectional extractions do not cause much discomfort after the procedure and require only simple analgesia such as Paracetamol (Panadol) and Ibuprofen (Nurofen) for several days, whilst some patients do not require much pain relief at all.
Surgical Extractions
Occasionally a tooth may fracture during the extraction, or due to a curved root structure, or because of its proximity to a nerve canal or sinus space, a tooth will require surgical removal. This can occur unexpectedly during the process of a simple extraction, or it can be planned prior to the extraction when looking at a patients x-ray. Or other people may require multiple teeth to be removed at the same time, and it is preferable to perform a combination of surgical and simple extractions to prevent unnecessary bone loss, prevent fractures, improve healing, and reduce post operative pain and discomfort.
Surgical extractions are often performed in the chair or they can be performed under sedation or a general anaesthetic in hospital. A surgical extraction involves making an incision into the gum and removing small pieces of bone and the tooth, and then placing sutures (stitches) to allow healing to occur.
Occasionally, the socket may be packed with a resorbable sponge to help blood clotting and stem the flow of any post operative bleeding, or it may be packed with a synthetic bone material to help the jaw bone recover quicker and prevent a loss of bone structure after the extraction. This is typically performed if a patient is considering implant replacement of the extracted tooth.
Sutures are typically removed 5 – 7 days after the surgical extraction and the patient may require stronger analgesics such as Panadeine Forte and a high dose Ibuprofen. Antibiotics may also be (but are rarely required to be) prescribed if there is a high risk that the patient may develop an infection.
Again, typically surgical extractions should not take excessive amounts of time, can be performed in around 15 – 20minutes (if not less), and should not be overly traumatic to the patient. Any surgical extraction should be no more complicated for the patient than having a moderate sized dental filling.
Medically Compromised Patients
As the population ages, so to does the number of patients with complex medical conditions that requires assistance from a dentist or oral surgeon. As mentioned previously, patients having cancer treatment, organ transplants, are taking multiple medications, are on anticoagulant treatment, have immunosuppression, diabetes, thyroid dysfunction, obesity, or even general old age and frailty all require additional care and attention.
Often these people do not require a specialist but rather are best treated with thorough pre-planning and preparation from a dentist with experience in treating medically compromised patients. Generally, any extractions will be performed in communication with the patients GP or treating specialist physician.
Patients on anticoagulant treatment for example should not cease their medications prior to having extractions performed, but rather plan to have a blood test taken several days before to assess their INR (bleeding time). Appropriate measures such as sutures, clotting packs, and transexamic acid mouthwashes, or fibrin glue can then be used by the dentist or oral surgeon to assist in bleeding control post operatively. Patients with INR’s up to 4.0 can be treated in this way.
In all cases, it is usually just a matter of having a consultation prior to any planned simple or surgical extractions so that a suitable treatment plan can be arranged and discussed with the patient, their GP and / or Physician. In this way, on the day of the surgery all appropriate steps and measures to care for the patient in a well controlled manner are thoroughly planned for.