Why Do We Have Wisdom Teeth
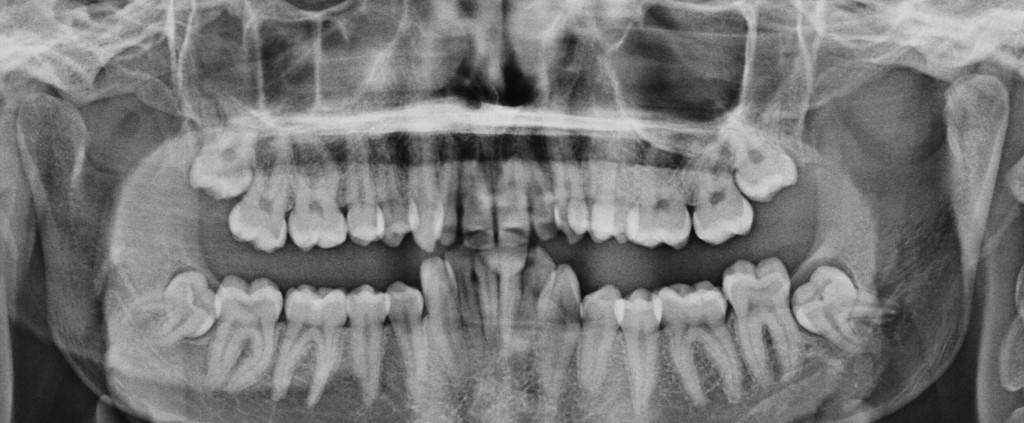
Wisdom teeth or 3rd molars are our last set of adult molar teeth that erupt into the mouth around the 18 years of age. Wisdom teeth were designed to enter the mouth when the other teeth had worn down from course diets such as eating from sand or coals as happened in primitive times. As the other teeth wore down, they would migrate forward leaving enough room for the wisdom teeth to erupt. We would therefore have a final set of grinding molar teeth to function until we passed away, typically at the age of 35.
Interestingly, many indigenous and aboriginal cultures do not routinely suffer from impacted wisdom teeth due to their course diets and larger facial bone structures.
Modern times and softer diets typically cause a large proportion of people to not have enough room in their jaws to allow wisdom teeth to erupt properly. Therefore, wisdom teeth become ‘impacted’. Unfortunately once wisdom teeth become impacted that often need to be removed to help prevent infections, inflammation of surrounding gum, jaw pain, decay and damage of adjacent molars, food trap, cysts, and dental crowding of other teeth.
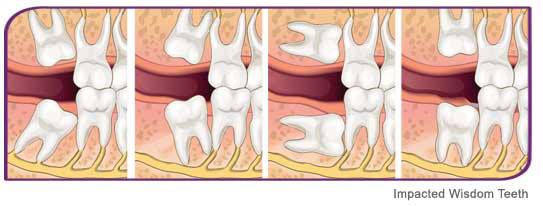
Impaction:
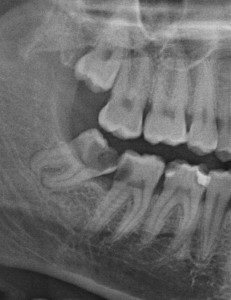
Wisdom teeth can be impacted vertically, horizontally, mesially (angled forward) and distally (angled backward).
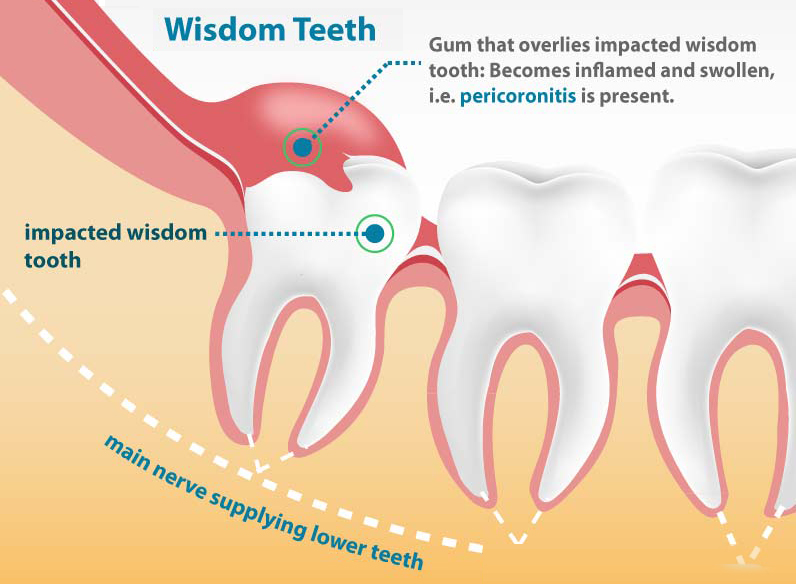
Impactions are generally the cause of all of the complications that can occur with wisdom teeth as described previously. Bacteria and food often will become trapped under the skin of the wisdom tooth and cause an infection or inflammation called “pericoronitis”. This becomes quite painful and is associated with a bad taste and bad smell. Often, episodes of pericoronitis will continue to occur for many months or years before a person will finally have the wisdom teeth removed.
This cycle of pain, infection, inflammation, food trap, and plaque accumulation underneath the skin and between the 2nd and 3rd molars can also lead to a chronic condition where the patient is not aware of the effect it is having on their immune system. The bacteria that is constantly present may contribute to tiredness, fatigue, a feeling of being run down, and regular colds and flus as the immune system is always ‘on the back foot’ trying to combat the low grade wisdom tooth infection. Many people after wisdom teeth surgery often comment some weeks later “I have so much more energy”.
In addition, chronic impacted wisdom teeth can cause decay in adjacent molars that often requires the 2nd molar to be extracted also as it is very difficult, if not impossible, for the general dentist to place a filling in this tooth once the wisdom tooth is removed.
Removal of Wisdom Teeth
The removal of wisdom teeth can be very straight forward or they may require surgical removal. Either way, surgery by an experienced practitioner helps make certain that the removal of wisdom teeth is an easy procedure that is not associated with undue pain, swelling, trauma, anxiety, or a long recovery period.
Every person seems to have a wisdom tooth horror story that really should be ignored by patients yet to have it done. The truth is like any procedure, there is a way of doing it, and there is a way of doing it well.
Like all surgical procedures however, there are risks and some minor swelling and post operative discomfort is to be expected. Using sound surgical skills and procedures, adequate pre and post surgery medications, excellent local anaesthetic techniques, and with experience, the removal of wisdom teeth and extractions of other teeth should not be overly traumatic or associated with extensive time, and delayed healing.
There are a variety of ways in which wisdom teeth can be removed. That is, in the chair under local anaesthetic either with or without various sedation techniques, under intravenous sedation, or in a hospital under a general anaesthetic. The method chosen is typically a combination of factors including the patients preferred option, complexity of the surgery, cost of hospital admission, and the presence of any anxiety or fear regarding the planned surgery. The actual technique for removing wisdom teeth should not differ depending on the location or complexity.
Sound surgical practice at all times includes pre-operative analgesia, good long-acting local anaesthetic, intraoperative anti-inflammatories, and post operative pain relief and anti-inflammatories for a period of 5 – 7 days, followed by a regular recall visit until healing is complete. At the Hobart Orofacial Pain and Special Needs Clinic we are uniquely qualified and experienced in providing surgical and sedation services not available at most general dental clinics. Please see our ‘Sedation’ section for further information.
Risks
The most common risks of removing wisdom teeth are:
- Minor swelling and discomfort
- Infections and dry sockets
- Sinus communications
- Temporary and permanent damage to nerves in the jaw and tongue
When surgery is performed properly, all of these risks are minimal and rarely occur. Complications with any procedure can happen no matter how simple and straight forward it appears from the outset however. When complications do occur, it is extremely important that they are managed properly and thoroughly from the time of surgery right through to the complete healing phase and resolution of the problem. That is why every person considering a surgical procedure such as wisdom teeth removal, should always seek an opinion from an experienced practitioner or specialist.